Can TMJ cause headaches? The real reason your head hurts
Millions of Australians live with recurring headaches and never find a satisfying answer. For a significant number of them, the answer has been in their jaw the whole time.
You have tried everything. You have tracked your water intake, cut out coffee, gone to bed earlier, taken the painkillers. The headaches keep coming. What nobody has asked you - and what might change everything - is: how is your jaw?
TMJ dysfunction is a well-recognised cause of secondary headaches, yet it remains one of the most commonly missed diagnoses in people with chronic head pain. In clinical practice, it is not unusual to see patients who have spent years being treated for tension headaches or migraines, whose symptoms improve dramatically once the jaw and neck are properly assessed and treated.
Yes - TMJ can absolutely cause headaches. Here is how.
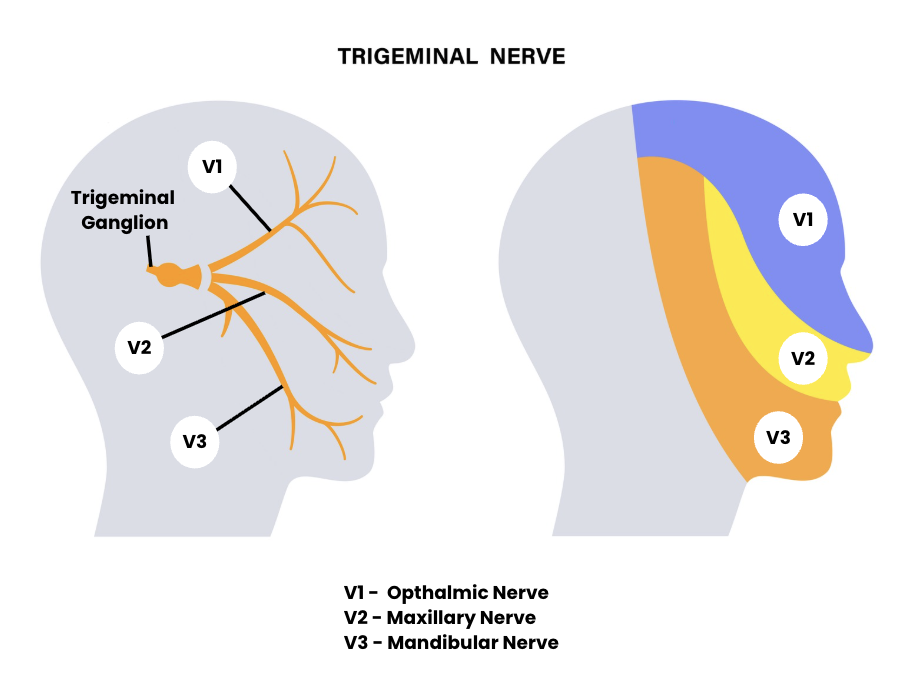
The temporomandibular joint sits immediately in front of your ear, right at the base of your skull. It shares nerve supply with a significant portion of the head and face via the trigeminal nerve - the largest cranial nerve in the body, responsible for sensation across the forehead, cheeks, jaw, and temples.
When the TMJ or its surrounding muscles are under load - through grinding, clenching, disc displacement, or postural strain - that irritation travels along the trigeminal nerve pathway and can refer pain directly into the head. This is called referred pain, and it is the same mechanism behind other well-known patterns like shoulder pain referring into the arm.
The trigeminal nerve has three branches covering the forehead, cheek, and jaw. When the TMJ is irritated, pain signals travel these pathways - which is why a jaw problem can produce headache pain in the temple, forehead or behind the eye.
Why doctors often miss it: TMJ headaches do not feel like they are coming from the jaw. They feel like a headache. Without specifically assessing the jaw and upper cervical spine, the connection is invisible - and patients end up cycling through migraine medications and tension headache treatments that only partially work, if at all.
The three mechanisms behind TMJ headaches
Masseter and temporalis muscle trigger points - The masseter (the main chewing muscle along the jaw) and the temporalis (the fan-shaped muscle covering the temple) are among the most powerful muscles in the body relative to their size. When they are chronically overloaded through clenching, grinding or poor jaw mechanics, they develop tight, irritable spots called trigger points. These refer pain directly into the temple, forehead, and behind the eye - and are among the most common sources of headache pain that gets mislabelled as tension or migraine.
Trigeminal nerve sensitisation - Chronic TMJ irritation can sensitise the trigeminal nerve over time, lowering the threshold at which it fires pain signals. This is part of why some people's headaches seem to have no obvious trigger. The system has become hypersensitive, and very little input is needed to produce significant pain.
Upper cervical spine involvement - The jaw and the upper neck are functionally inseparable. Dysfunction at C1, C2 and C3 - the top three vertebrae - refers pain into the head through the trigeminal-cervical complex. Most people presenting with TMJ headaches also have restricted upper cervical movement, and addressing both is nearly always necessary for lasting resolution.
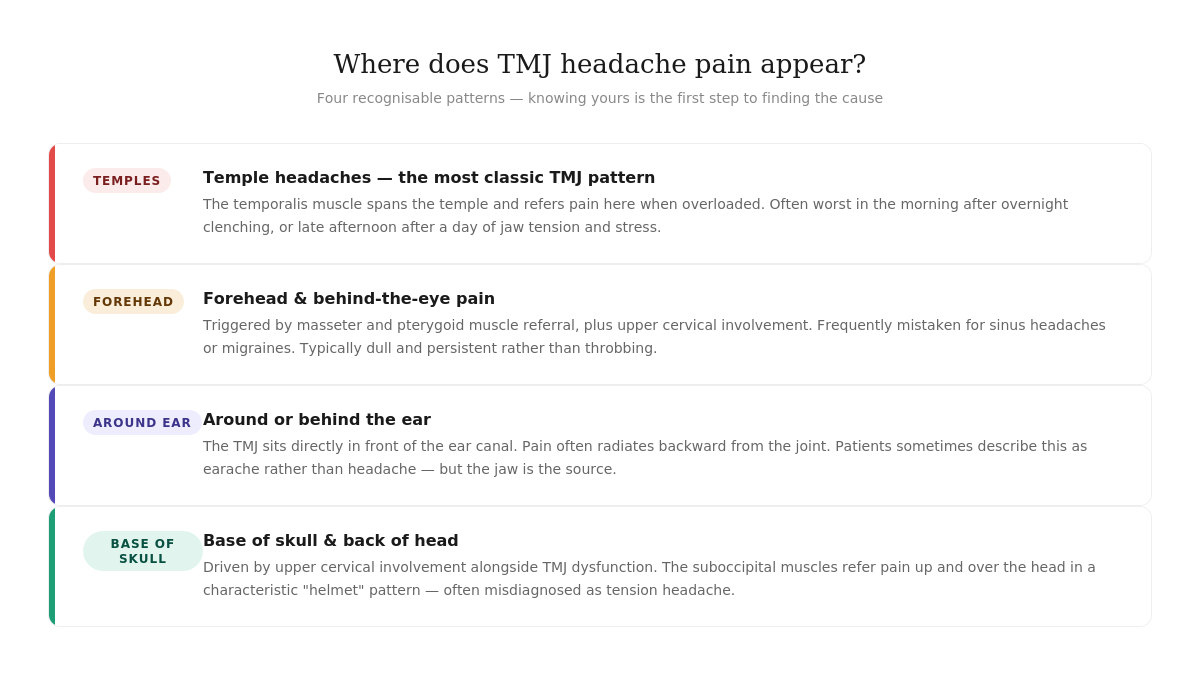
Where does the pain actually appear?
TMJ-related headaches have recognisable patterns. Knowing which type you are experiencing is one of the most useful clues in identifying the jaw as a source:
How to tell if your headaches might be jaw-related
There is no single definitive test you can do at home, but these patterns are strong indicators that the jaw and neck deserve assessment:
Important: Not all headaches are TMJ-related, and some require urgent medical assessment. If your headaches are sudden and severe, associated with vision changes, weakness or confusion, or are the worst headache of your life, seek emergency medical care immediately. This post is about chronic, recurrent headaches - not acute or sudden-onset head pain.
Where osteopathy fits in
Because TMJ headaches involve the jaw, the upper cervical spine, and the nervous system simultaneously, they respond best to treatment that addresses all three together. Osteopathic assessment looks at how the jaw is tracking, where restrictions exist in the upper neck, how the suboccipital muscles are loading and what postural or lifestyle factors are keeping the system under tension.
For many patients, this is the first time anyone has assessed their jaw and neck as a system in the context of their headaches - and the results can be striking. Headaches that have been present for years often begin responding within a handful of sessions once the underlying mechanical drivers are identified and treated.
This does not mean every headache will resolve completely with osteopathic care alone. But for people whose headaches have a jaw and neck component - which in clinical experience is a significant proportion of those with chronic tension or unclassified headaches - it is a piece of the puzzle worth exploring.
The bottom line
If you have had recurring headaches for months or years without a satisfying explanation, your jaw and upper neck deserve a proper assessment. TMJ dysfunction is a recognised, treatable cause of chronic headaches - and one of the most commonly overlooked. You do not have to keep managing the symptom when the cause might be identifiable and addressable.
Still looking for answers?
Your headaches might
finally make sense
If you have been living with recurring headaches and your jaw and neck have never been properly assessed, a single osteopathic consultation could give you the clarity you have been missing. We assess the jaw, neck, and nervous system together - because that is where the answers usually are.
Jaw & neck assessed together - No referral required - Chronic headache experience
Sources: Migraine & Headache Australia; Australian Dental Journal; Juniper Publishers (2019); Sage Journals - TMD and Headache Systematic Review (2022); Australian Physiotherapy Association.
This post is for general information only and does not constitute clinical advice. If you experience sudden, severe, or unusual headaches, please seek urgent medical attention.